23 October 2019

Use of MRI may prevent an Alzheimer’s misdiagnosis in seniors with memory loss
Los Angeles, CA, USA – A UCLA-led study finds that, with the use of magnetic resonance imaging (MRI) scans, it is possible to distinguish between memory loss caused by Alzheimer’s disease and traumatic brain injury.
Researchers from UCLA, along with colleagues at Washington University in St. Louis, say the finding is important because it could help prevent a misdiagnosis of Alzheimer’s disease, which can be devastating for patients and their families. One study found that as many as 21 percent of older adults with dementia may be misdiagnosed with Alzheimer’s disease. A misdiagnosis can result in patients not receiving the appropriate treatment, and prevents them from participating in clinical trials that could improve their overall care.
The current study, published in the Journal of Alzheimer’s Disease, involved 40 UCLA patients with an average age of just under 68, who had suffered traumatic brain injury, or TBI, and then later developed memory problems. According to the US Centers for Disease Control and Prevention 2.87 million Americans experienced TBI in 2014, with the rates highest for people age 75 or older. Children age 4 and younger, and adults age 65 and older were most likely to suffer serious brain injuries after a fall.
“We already knew that MRIs can reveal subtle abnormalities in patients with neurological disorders, such as Alzheimer’s,” said Dr. Somayeh Meysami, lead author of the study in the department of neurology at the David Geffen School of Medicine at UCLA. “The purpose of our study was to evaluate whether MRI also could reveal distinct abnormalities in traumatic brain injury. And, if we could identify such a pattern, it would lead to improved diagnosis of TBI-related memory loss from other causes of dementia.”
Using a software program to analyze the MRI scans, the study revealed that TBI caused the most damage to a brain region known as the ventral diencephalon, with the least amount of atrophy occurring in the hippocampus, said study author Dr. Cyrus Raji, an assistant professor of radiology at Washington University in St. Louis. The ventral diencephalon is associated with learning and emotions, whereas the hippocampus is involved in memory and emotions. The hippocampus also is the region of the brain that is most impacted by Alzheimer’s disease.
“The method we used to measure brain volumes in these individuals is useful because it can be applied on the same type of MRI scans we obtain in the clinic with no special type of imaging required,” Dr. Raji said.
The Alzheimer’s Association estimates that up to 40 percent of dementias are caused by conditions other than Alzheimer’s disease.
“Our study offers further evidence that not all memory loss is caused by Alzheimer’s disease,” he said. “It can attributed to TBI, as well as other dementias and neurodegenerative disorders,” said Dr. Mario Mendez, a professor-in-residence of neurology, psychiatry and biobehavioral Sciences at the David Geffen School of Medicine at UCLA.
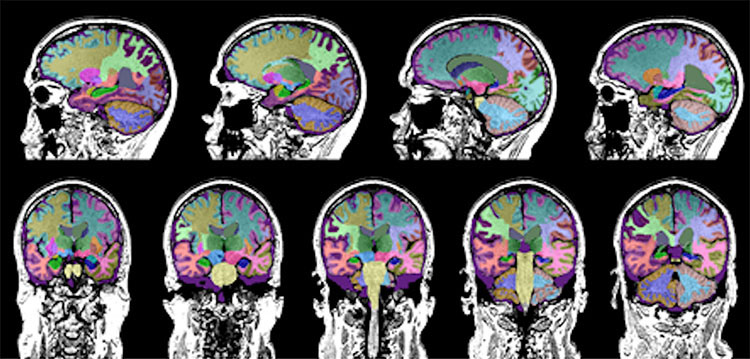
Caption: Color coded segmentation from the Neuroreader software program used for quantifying brain volumes in persons with TBI in the study.
###
NOTES FOR EDITORS
Full study: "MRI Volumetric Quantification in Persons with a History of Traumatic Brain Injury and Cognitive Impairment" by Somayeh Meysami, Cyrus A. Raji, David A. Merrill, Verna R. Porter, Mario F. Mendez (DOI: 10.3233/JAD-190708), published online in the Journal of Alzheimer's Disease in advance of the publication of Volume 72, Issue 1. The article is online at: content.iospress.com/articles/journal-of-alzheimers-disease/jad190708.
Media Contact
Marrecca Fiore
mfiore@mednet.ucla.edu
+1 310-267-7095
About the Journal of Alzheimer's Disease
Now in its 22nd year of publication, the Journal of Alzheimer's Disease (JAD) is an international multidisciplinary journal to facilitate progress in understanding the etiology, pathogenesis, epidemiology, genetics, behavior, treatment, and psychology of Alzheimer's disease. The journal publishes research reports, reviews, short communications, book reviews, and letters-to-the-editor. Groundbreaking research that has appeared in the journal includes novel therapeutic targets, mechanisms of disease, and clinical trial outcomes. JAD has a 2018 Journal Impact Factor of 3.517 according to Journal Citation Reports (Web of Science Group, 2019) and is published by IOS Press. j-alz.com







